Hernias in women are very difficult to diagnose. These are very small and very hard to identify. As women typically Read More...
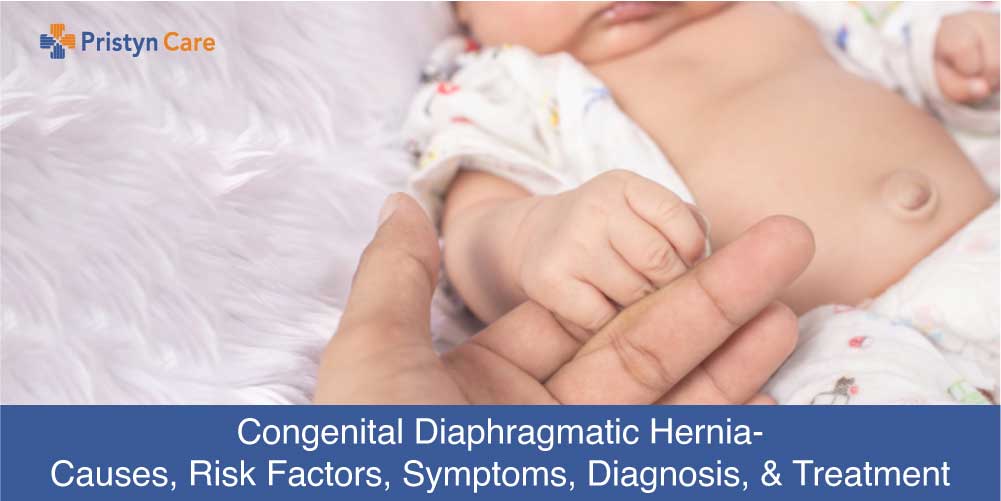
Congenital Diaphragmatic Hernia- Causes, Risk Factors, Symptoms, Diagnosis, and Treatment
1 month agoWhat is Congenital Diaphragmatic Hernia
The Congenital Diaphragmatic Hernia is simply a birth defect that occurs i Read More...
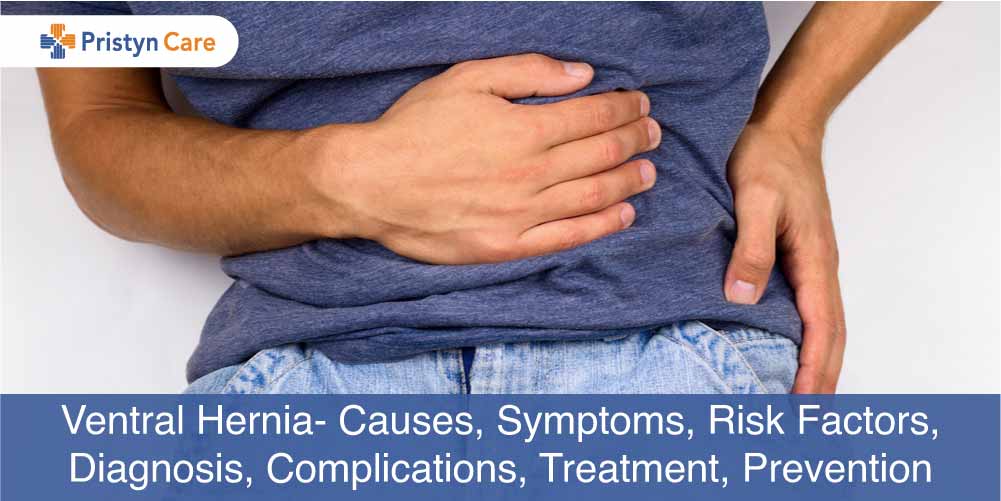
Ventral Hernia- Causes, Symptoms, Risk Factors, Diagnosis, Complications, Treatment, Prevention
1 month agoWhat is Ventral Hernia
The hernia that occurs along the vertical center of the abdomen is a ventral hernia. It can Read More...
What is Femoral Hernia?
A femoral hernia occurs when an organ displaces from its original place through a weak p Read More...
Spigelian Hernia Symptoms, Causes, Treatment
1 month ago What is a Spigelian Hernia?
Spigelian hernia is the hernia that forms through the Spigelian aponeurosis. S Read More...
Spermatocele, a benign cyst found in the epididymis, affects approximately 30% of men in their lifetime. While caus Read More...
What Size Hernia Needs Surgery?
1 month agoIntroduction:
Hernias are persistent protrusions that occur when an organ or fatty tissue squeezes through a weak Read More...
Is Hernia Curable Without Surgery?
1 month agoHernias are a common ailment, affecting millions worldwide, prompting the question: is hernia curable without surge Read More...
Stiff Neck Causes, Symptoms, And Treatment
1 month agoA stiff neck is a common problem and affects 10% of the population. The stiffness, if not treated, can spread to ot Read More...
Which Doctor to Consult for Inguinal Hernia?
1 month agoIf you suspect you have a hernia, your first action should be to find the best doctor and schedule an appointment. Read More...
Which Doctor to Consult for Hernia
1 month agoWhen it comes to hernia repair treatment, the process of finding the best laparoscopic surgeon can be stressful. Ta Read More...
Hydrocele – Symptoms and Causes
1 month agoWhat is Hydrocele?
Hydrocele is a urological condition that is common in newborns. However, it can also affect adu Read More...