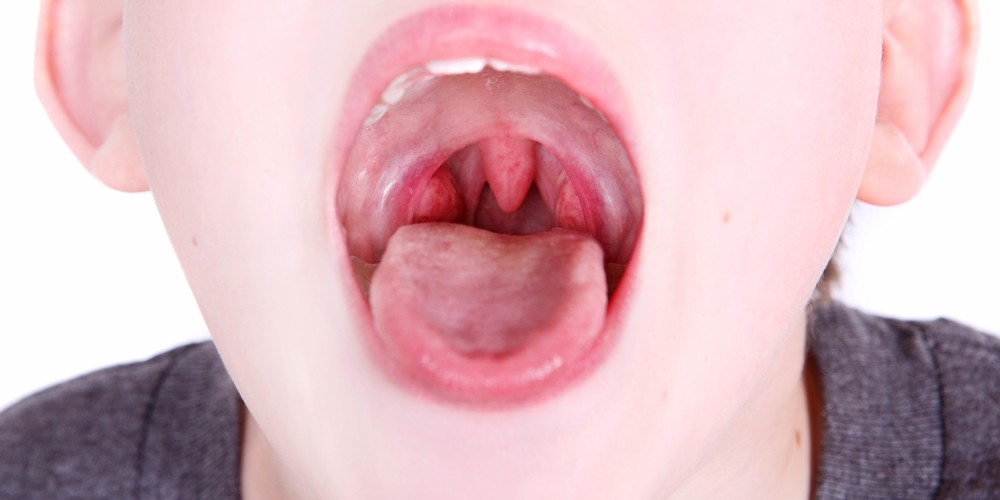
According to Dr. Siddhartha Vashishtha, ENT doctor from Pristyn Care, “The most common cause of a sore throat is Read More...
What is Phlegm in the throat?
Some mucus in the airways can protect and moisturize the tissues. Phlegm is a type o Read More...
10 Home Remedies For Tonsils (Tonsillitis)
7 months agoMost of the time the patient knows that he or she has tonsillitis. Tonsillitis usually occurs in young children but Read More...
A sore throat can make some situations uncomfortable. Other than a sore throat, some other symptoms could be pain o Read More...