
Delhi
USFDA-Approved Procedure
Patient Centric Approach
1-day Hospitalization
Cost Effective Treatment

We at Pristyn Care Perform 5 types of treatment as follows:
Q-switched lasers emit nanosecond pulses that break up melanin granules without damaging the surrounding tissue in the treatment area. Dermatologists set the wavelength to either 532 nm or 1064 nm, depending on the skin type. The procedure addresses black vaginal whitening by targeting the deep dermal pigment. Sessions last between 15 and 30 minutes. Practitioners apply cooling gel to prevent thermal injury.
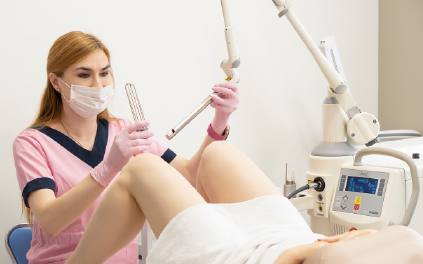
Prescription formulations contain hydroquinone (2 to 4%), kojic acid, or azelaic acid that inhibit tyrosinase enzyme activity in melanocytes. These agents slow melanin synthesis in dark private area skin. Dermatologists prescribe creams for mild to moderate pigmentation and monitor for irritation every two weeks. Treatment duration spans 8 to 12 weeks.

Glycolic acid (30 to 50%) or trichloroacetic acid peels dissolve the stratum corneum, removing pigmented cells from the surface. Dermatologists apply peels to brighten vaginal area concerns after patch testing. The procedure exfoliates dead skin and reveals lighter layers beneath. Peeling starts 48 hours post-application and completes within five days. Dermatologists recommend 4 to 6 sessions for sustained results.

Automated microneedling devices create controlled micro-injuries that trigger collagen production and accelerate cellular renewal in treated skin. Practitioners infuse tranexamic acid or vitamin C serums during the procedure. This method reduces black spots on vagina and stimulates dermal regeneration. Each session lasts 30 minutes. Patients require 4 to 5 treatments monthly. The technique suits sensitive genital skin prone to irritation.

Dermatologists integrate laser sessions with topical agents and chemical peels for accelerated lightening in resistant pigmentation cases. Laser breaks down deep pigment. Peels remove surface layers. Creams maintain results between sessions. This approach effectively treats stubborn dark genital areas, including cases of acanthosis nigricans in the genital area.

Q-switched lasers emit nanosecond pulses that break up melanin granules without damaging the surrounding tissue in the treatment area. Dermatologists set the wavelength to either 532 nm or 1064 nm, depending on the skin type. The procedure addresses black vaginal whitening by targeting the deep dermal pigment. Sessions last between 15 and 30 minutes. Practitioners apply cooling gel to prevent thermal injury.

Prescription formulations contain hydroquinone (2 to 4%), kojic acid, or azelaic acid that inhibit tyrosinase enzyme activity in melanocytes. These agents slow melanin synthesis in dark private area skin. Dermatologists prescribe creams for mild to moderate pigmentation and monitor for irritation every two weeks. Treatment duration spans 8 to 12 weeks.

Glycolic acid (30 to 50%) or trichloroacetic acid peels dissolve the stratum corneum, removing pigmented cells from the surface. Dermatologists apply peels to brighten vaginal area concerns after patch testing. The procedure exfoliates dead skin and reveals lighter layers beneath. Peeling starts 48 hours post-application and completes within five days. Dermatologists recommend 4 to 6 sessions for sustained results.

Automated microneedling devices create controlled micro-injuries that trigger collagen production and accelerate cellular renewal in treated skin. Practitioners infuse tranexamic acid or vitamin C serums during the procedure. This method reduces black spots on vagina and stimulates dermal regeneration. Each session lasts 30 minutes. Patients require 4 to 5 treatments monthly. The technique suits sensitive genital skin prone to irritation.

Dermatologists integrate laser sessions with topical agents and chemical peels for accelerated lightening in resistant pigmentation cases. Laser breaks down deep pigment. Peels remove surface layers. Creams maintain results between sessions. This approach effectively treats stubborn dark genital areas, including cases of acanthosis nigricans in the genital area.



See the remarkable transformations for yourself | Our 'Before & After' Slider highlights the impact of Genitals Whitening.
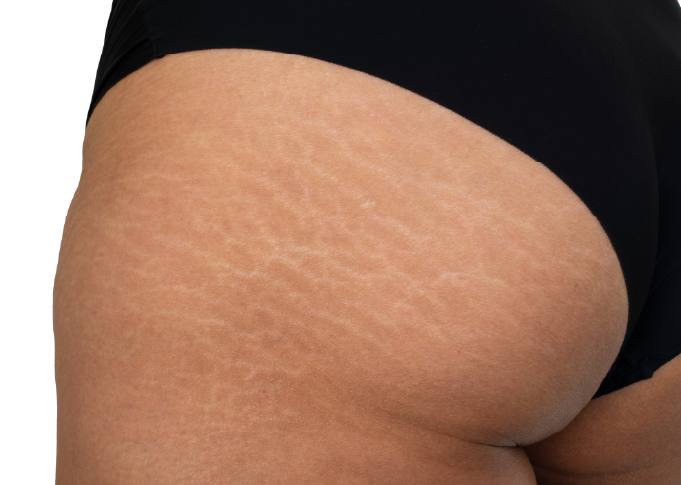
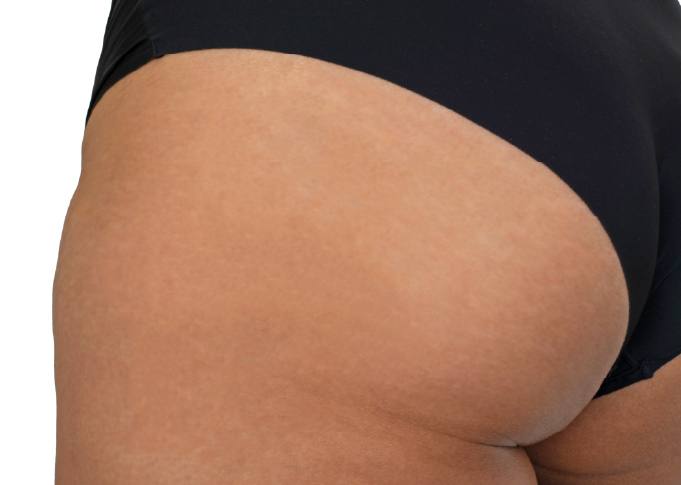





.png)

Topical anesthetics eliminate pain before treatment begins. Patients experience pressure or warmth during laser pulses or peel application.
Mild pigmentation requires 3 to 4 treatments. Severe dark genitals treatment in Delhi cases need 5 to 7 sessions spaced monthly.
Melanocytes remain active, so pigmentation recurs without friction management, hormonal balance, and quarterly maintenance applications at the clinic.
Pregnant or breastfeeding women, active genital infections, keloid-prone individuals, and those on photosensitizing medications should postpone black vagina whitening until conditions resolve.
Acanthosis nigricans in the genital area respond to combination therapy that lightens pigmentation while managing underlying insulin resistance through medical consultation and metabolic control.
Estrogen and progesterone spikes during menstruation or pregnancy increase melanocyte activity in genital skin. This leads to more pigment production. Tight clothing rubs against the labia and inner thighs. This friction results in post-inflammatory hyperpigmentation. Insulin resistance causes the body to make too much melanin in skin folds, which shows up as acanthosis nigricans in the genital area. Aging also slows down cell turnover, letting pigmented cells accumulate.
Type 2 diabetes and prediabetes raise insulin levels. This activates insulin-like growth factor receptors on keratinocytes in skin folds. As a result, the skin thickens and darkens in areas like the genital folds, neck, and armpits. Patients with PCOS also have high insulin levels, which leads to similar changes in skin color. Obesity amplifies insulin resistance, worsening acanthosis nigricans the genital area. Certain medications (corticosteroids, niacin) induce pigmentation as a side effect. Rare endocrine tumors secrete hormones that darken skin.
Weight control lessens friction between the thighs and prevents insulin resistance, which can lead to acanthosis in the genital area. Breathable cotton underwear also allows air to flow and helps prevent moisture buildup. Regular gynecological exams can spot early pigmentation changes related to hormonal imbalances. Diabetes control through medication and diet prevents causes of acanthosis nigricans progression.
Sudden darkening accompanied by itching or pain requires immediate dermatological assessment for infection or allergic reaction. Asymmetrical pigmentation spreading beyond genital folds needs biopsy to rule out malignancy. Persistent black spots on vagina unresponsive to home care warrant professional evaluation. Bleeding or discharge from darkened areas indicates infection requiring antibiotic treatment.
.svg)