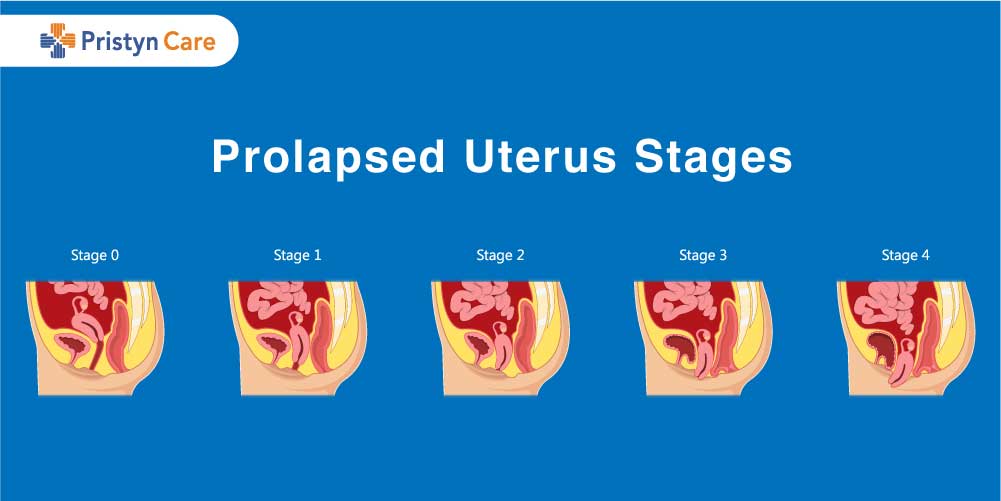
Uterine prolapse occurs when the uterus descends towards or into the vaginal canal. It occurs when the pelvic floor muscles and ligaments get weak and can no longer support the uterus. In some cases, the uterus can even protrude from the vaginal opening.
Complications can at times occur in case of uterine prolapses, such as ulceration of exposed tissues or prolapse of other pelvic organs including the bladder or the rectum. Among females aged 55 years and above, uterine prolapse is one of the most common reasons for undergoing a hysterectomy.
Risk factors for uterine prolapse include having a high BMI (body mass index), menopause, pregnancy, and vaginal childbirth. Symptoms of uterine prolapse include urinary leakage or stress urinary incontinence, discomfort in the pelvis, and severe and/or frequent lower back pain. Kegel exercises are considered very helpful for treating mild stages of uterine prolapse.
Table of Contents
Stages of uterine Prolapse
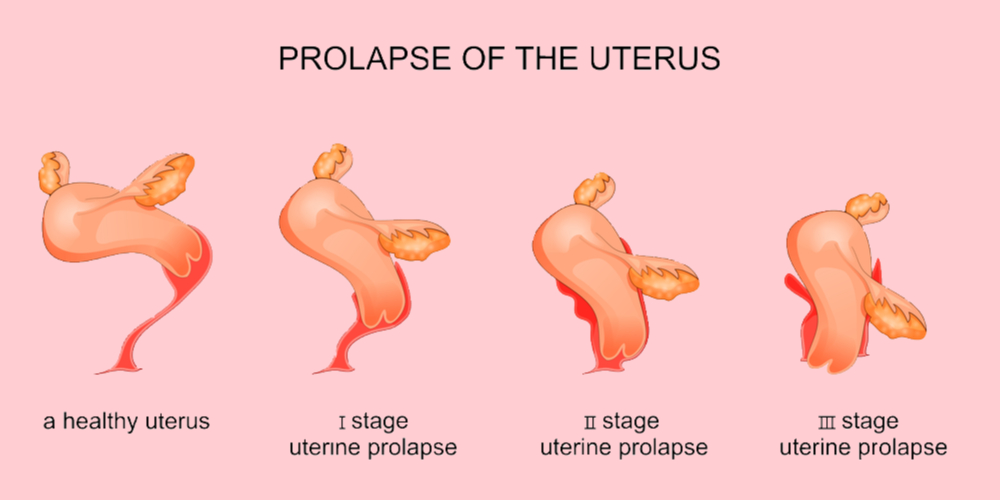
Uterine prolapse can be classified as incomplete or complete uterine prolapse-
- Incomplete uterine prolapse- In this stage, the uterus is partially displaced into the vaginal canal but does not protrude.
- Complete uterine prolapse- In this stage, a portion of the uterus protrudes from the vagina.
The condition of uterine prolapse is graded by the severity and how far the uterus has descended into the vaginal canal-
- 1st grade of uterine prolapse- The uterus descends to the upper vagina
- 2nd grade of uterine prolapse- The uterus descends to the introitus
- 3rd grade of uterine prolapse- The cervix descends outside the introitus
- 4th grade of uterine prolapse- Both the cervix and uterus descend outside the introitus
More severe cases of uterine prolapse may also be there, which may need immediate surgery, but in the early stages, exercises can help treat the condition and get relief.
Causes of uterine prolapse
Weakened pelvic floor muscles are the most common cause of uterine prolapse. Pelvic floor muscles can become weak for a number of reasons:
- Pregnancy
- Vaginal childbirth
- Factors related to vaginal delivery, such as trauma or delivering a heavy baby
- Menopause
- Frequently lifting heavy weights or objects
- Chronic coughing
- Straining during bowel movements
- History of pelvic surgery
- Genetic factors leading to weak connective tissue
Symptoms of uterine prolapse

Symptoms of uterine prolapse vary depending on how severe the condition is. Typical symptoms may include the following-
- Pelvic heaviness
- Pulling or aching sensation in the vagina, which gets worse during periods or sex
- Moist, pink tissues bulging from the vagina
- Spotting or bleeding between periods
- Increase in vaginal discharge
- Frequent urination
- Sexual discomforts like
- Painful sexual intercourse, urine leakage during sex and inability to reach orgasms.
- Stress Urinary Incontinence or urinary leakage
- Bladder infections
- Frequent urinary tract infections (UTIs)
- Bowel movement problems, such as constipation
- Lower back pain
- Feeling like sitting on a ball or feeling that something is falling out of the vagina
- Weak vaginal muscles and tissues
In mild cases of uterine prolapse, the female might nor observe severe or discomforting symptoms. Symptoms that appear sometimes often get worse towards the end of the day.
Diagnosis
A gynecologist will ask the female about symptoms she is having and accordingly perform a physical examination. While examining the pelvis, the gynecologist will evaluate vaginal tone and organ placement. MRI or an ultrasound may be suggested to help assess the severity of the uterine prolapse.
Home Remedies for early stages of uterine prolapse
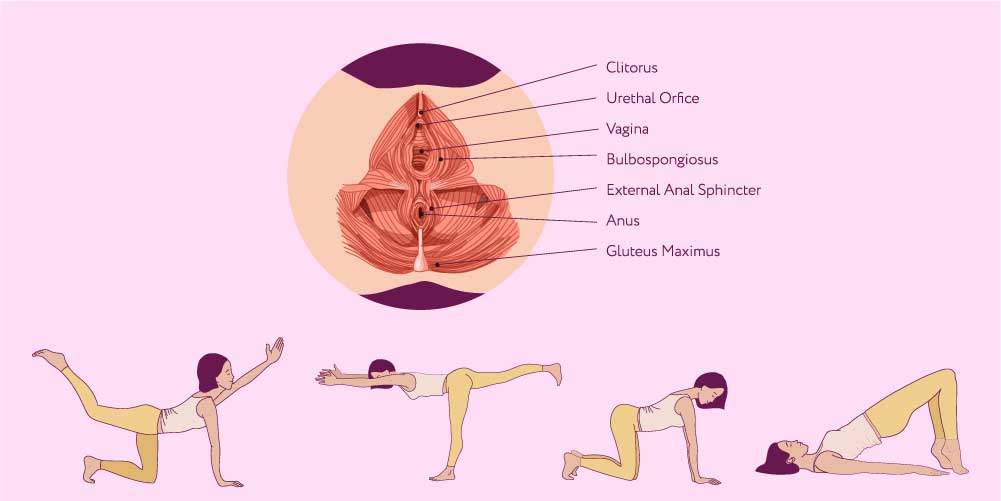
Treatment or home remedies of uterine prolapse depend on the stage and severity of the condition. Some strategies can readily reduce the risk of uterine prolapse developing or stop it from worsening in the very initial phase.
The strategies or self-care tips include-
- Perform Kegels regularly and correctly
- Prevent and treat constipation
- Avoid heavy lifting
- Use correct body mechanics, if weight lifting is necessary
- Manage chronic coughing
- Maintain a healthy weight
- Consider estrogen replacement therapy if you are in menopause
Medical Treatment

In cases of mild uterine prolapse, the female can reverse and treat the condition by doing pelvic-muscle strengthening exercises such as Kegels. Undiagnosed or if left untreated, the stage and severity of uterine prolapse increase over time.
Advanced and severe cases of prolapsed uterus mostly do not respond to exercises or hormonal therapy. In such cases, the female needs to undergo surgery or vaginal tightening treatment to improve and cure the prolapsed uterus.
Prolapse up to the 3rd degree can spontaneously resolve by working with your gynecologist. More severe cases require medical treatment or even surgery.
Medical options for uterine prolapse include:
Vaginal pessary: It is a vaginal device that supports the uterus and keeps it in the proper position. It is essential to follow the instructions on removal, insertion and taking care of the pessary. In cases of severe uterine prolapse, a pessary can lead to irritation, ulceration, or sexual problems. Discuss with your gynecologist if this treatment is right for you.
Surgery: Surgical repair of the prolapsed uterus can be performed through the abdomen or vagina. Surgical options may involve skin grafting, use of donor tissue or other material to provide uterine suspension. A hysterectomy may be recommended in case of severe cases and if the female has completed her family.
If future pregnancies are intended, surgery may not be recommended for the female, due to the risks of or effects of surgical repair. A female can undergo vaginal tightening to strengthen and tighten her vaginal tissues, which can readily solve the problem of uterine prolapse.







