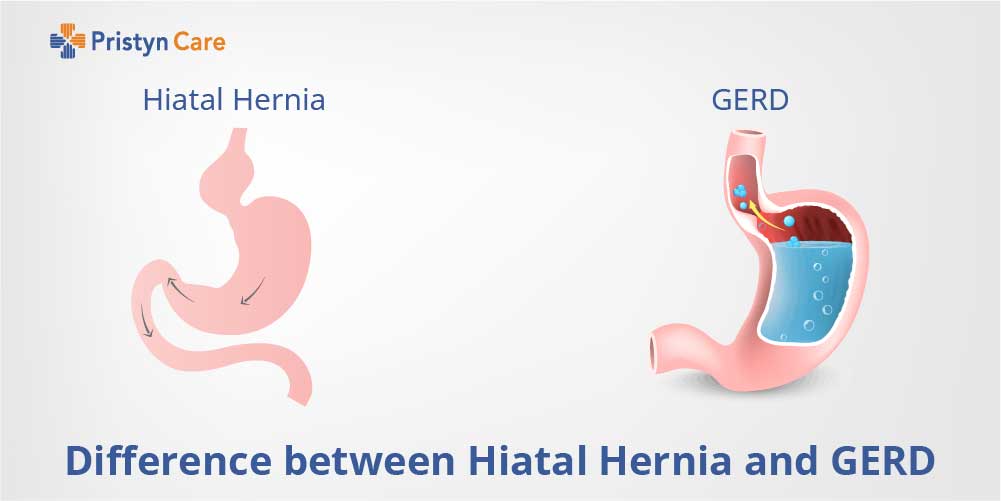
Hiatal hernia and gastroesophageal reflux disease are two different terms, but to understand the difference between Hiatal hernia and Gastro esophageal reflux disease, it’s important to understand the role of hiatal hernia in Gastroesophageal reflux disease.
What do you mean by the term Hiatal hernia?
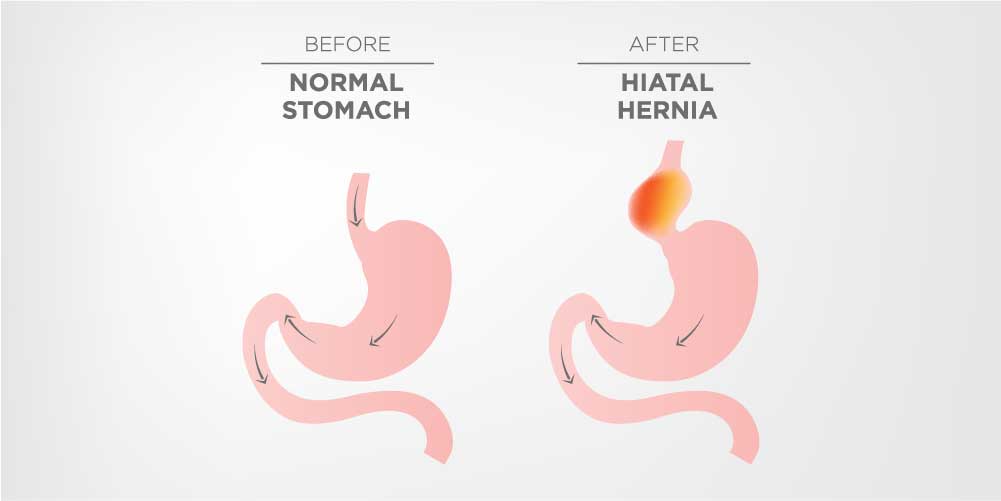
Hiatal hernia is a condition where the abdominal constituents like the gastroesophageal junction and certain parts of the stomach displace proximally above the region of the diaphragm that connects through the areas of esophageal hiatus directly into the mediastinum.
Table of Contents
Symptoms of Hiatal hernia:
Hiatal hernias initially do not cause any symptoms and pain like symptoms can be noticed only when the protrusions of the stomach become large. Smaller hernias of these types are most often asymptomatic. Larger size Hiatal hernias allow the undigested food and acids of the stomach to reflux directly into the esophagus displaying the standard symptoms of GERD. Some of the symptoms of Hiatal hernia include
- Heartburn
- Trouble swallowing food due to obstruction
- Chest pain which intensifies with bending over or lying down
- Fatigue
- Abdominal pain
- Frequent burping
- Sore throat
Types of Hiatal Hernias
There are two major types of hiatal hernia:
- Sliding hiatal hernia and
- Paraesophageal hiatal hernia
Depending upon how one would subdivide the para esophageal Hiatal hernias, it can be further categorized into three or four types, and which are explained as follows:
Type I
Type I hiatal hernia or sliding hiatal hernia is the most common type of all Hiatal hernias which results from the general weakening of the cardia muscles and ligaments. Sliding hernia or type I hernia sac consists of retroperitoneal fat that is protruded into the esophageal hiatus. This causes the cardia muscles and ligaments to slide upward into the posterior mediastinum causing stomach contents to pass into the esophagus and thus results in gastroesophageal reflux disease.
Type II
Type II hiatal hernia is the form of para esophageal hernia in which part of the gastric fundus protrudes out and forms a sac above the diaphragm. The peritoneal sac formed in this type of hernia in the esophageal hiatus fails to return to its original position and remains bulging like a sac into the posterior mediastinum.
Type III
Type III hiatal hernia is generally the mixture of type I and II hiatal hernia. In this type, along with the paraesophageal hiatal hernia, the Gastroesophageal junction is not fixed but displaced above the areas of diaphragm.
Type IV
It is a type of giant para esophageal hiatal hernia (type IV). This type of hernia is classified by its size, where the hernia sac may include more than one-third to one-half of the stomach. Type IV hernias include upper abdominal organs of the body like the thorax, colon, small intestine, omentum, liver, and spleen. It is an aggravated form of type III hiatal hernia.
What is Gastro esophageal reflux disease (GERD)?
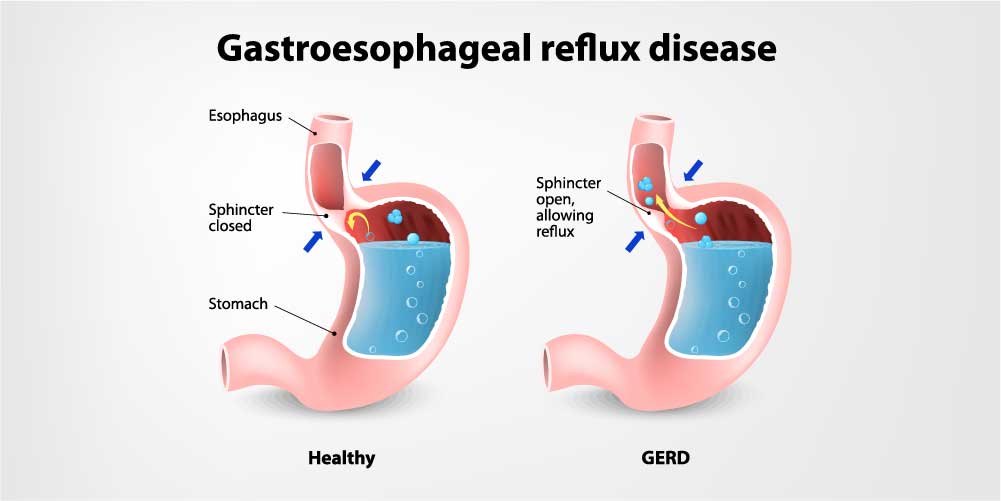
This is a chronic gastrointestinal condition that occurs when the stomach acid flows back into the esophagus irritating the lining of the esophagus connecting your mouth and stomach. Symptoms include heartburn, pain in the chest, dysphagia, laryngitis, and disturbed sleep. GERD may be manageable through dietary interventions and lifestyle changes. But more severe conditions may need surgery to ease the symptoms. (Also Read: Difference Between GERD and Heartburn- Symptoms and Treatment )
Etiology behind GERD
When you consume food a circular band of muscles allows food to enter the stomach. This band is called sphincter which relaxes to allow food into the stomach and then closes once the food is inside the stomach. The sphincter becomes weak in the person suffering from GERD which causes the backflow of stomach acidic contents into your esophagus irritating the mucosa.
Causes of GERD
GERD can result due to Obesity, presence of hiatal hernia, pregnancy, and delayed stomach emptying due to high-fat foods consumption or fried foods.
Difference between hiatal hernia and gastro esophageal reflux disorder
Hiatal hernia is a protrusion of gastrointestinal junction and stomach parts towards the diaphragm. Whereas, GERD is a condition where the acidic contents of the stomach pass into the esophagus. This may be due to the reduced pressure on the lower esophageal sphincter muscle.
A hiatal hernia can be a cause of gastro esophageal reflux disorder. But GERD is not a cause of hiatal hernia. For instance, hiatal hernia is related to the anatomic distortion of gastro esophageal junction, stomach parts and maybe also involved in the physiological dysfunction of the LES that may result in acid reflux into the esophagus. Hiatal hernias can be a contributing factor to the chronic nature of gastro esophageal reflux disease.
However, it is also important to note that Hiatal hernias are not the sole contributors of GERD and other factors may also be associated with cause GERD irrespective of hiatal hernia.
Hiatal Hernia | Gastro esophageal disease (GERD) |
| Hiatal hernia may develop due to chronic acid reflux | GERD may develop irrespective of hiatal hernia and is not necessarily associated with Hiatal hernia. |
| Shortness of breath may occur in people suffering from hiatal hernia | There is no association with symptoms such as shortness of breath |
| Vomiting, Gastrointestinal bleeding or passing of black stools may develop | A person suffering from GERD does not experience vomiting and GIT bleeding. |
| Noticeable chest and abdominal pain | Chest pain is a common symptom of GERD |
Treatment for hiatal hernia and GERD
Symptoms of Hiatal hernia and GERD are easily manageable through dietary changes when the conditions are not so worse.
- Eating smaller meals throughout the day
- Avoid foods that trigger heartburn (Also Read: Diet for Hiatal Hernia Patients )
- Do not sleep immediately after consuming food and sleep after 3 hours at least
- Avoid smoking and alcohol
Another treatment option may include Surgery
The doctors suggest surgery only when the conditions are worse, and when medications, lifestyle and dietary alterations fail to respond. Surgery is performed under conditions that have severe esophagitis, suffering from pneumonia due to stomach acids, severe heartburn, and a person with an esophageal stricture.
Types of surgery
Open repair surgery
This surgery involves a large incision on the abdomen under general anesthesia. In this procedure, the surgeon pulls your stomach and wraps it around the lower portion of the esophagus to make the sphincter tight.
Laparoscopic surgery
It is a minimally invasive technique when compared to open repair surgery. In this surgery, the surgeon makes 2-3 incisions on the abdomen and inserts instruments with a laparoscope on the site. The surgeon then pulls your stomach with the help of small sterilized instruments and wraps the upper part of the stomach towards the lower end of the esophagus producing tighter sphincter. (Also Read: Role of Laparoscopy to Treat Hernia Effectively)
Endoscopic fundoplication
The surgeon places small clips onto the stomach at the place where the esophagus meets the stomach. The procedure is guided with an endoscope that directs the surgeon to the site by projecting a video of the GIT tract. Endoscopic fundoplication is the least invasive procedure.
Final Words
A person suffering from hiatal hernia may suffer from GERD. But many people experience hiatal hernia without GERD. The relationship between these two conditions is relatively intertwined however; there exists a close relationship between hiatal hernia size and incidence of GERD.
Also Read:







